The Dual Nature of Iron in Relation to Cancer: A Review
AUTHORS
Sayed Hossein Davoodi 1 , 2 , Yasaman Jamshidi-Naeini 2 , Saeideh Esmaeili 3 , Sara Sohrabvandi 3 , Amir M. Mortazavian 3 , *
1 Cancer Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran
2 Faculty of Nutrition Sciences and Food Technology, Shahid Beheshti University of Medical Sciences, Tehran, Iran
3 Department of Food Science and Technology, National Nutrition and Food Technology Research Institute, Faculty of Nutrition Sciences and Food Technology, Shahid Beheshti University of Medical Sciences, Tehran, Iran
How to Cite: Hossein Davoodi S, Jamshidi-Naeini Y, Esmaeili S, Sohrabvandi S, Mortazavian A M. The Dual Nature of Iron in Relation to Cancer: A Review, Int J Cancer Manag. 2016 ; 9(6):e5494. doi: 10.17795/ijcp-5494.
Abstract
Background: Although iron is essential for all cells, it could be potentially hazardous. This is mostly due to iron participation in oxidation-reduction reactions. In terms of cancer risk, the role of both iron deficiency and overload can be studied in two directions, protective or therapeutic effects, and carcinogenic effects.
Materials and Methods: PubMed, Science direct, Ovid, Proquest, Medline, and Google scholar databases were used to obtain articles identified by using the key words “Iron”, “Iron deficiency”, “Iron overload”, “Cancer”, and “Neoplasm” without any time limit. The relevance of studies was identified by reviewing the titles and the abstracts. 185 articles published in English, including experimental, observational, molecular and cellular studies were reviewed.
Results and Conclusion: Considering the dual nature of iron, maintaining an optimal iron level in the body is important. This can be achieved when regulatory mechanisms of body iron level work properly and the amount of iron input is within the physiological range. Current evidence generally supports this possibility that higher animal-derived (heme) iron may increase the risk of some cancers. The release of iron or nitrosyl heme from iron complexes during some processing of meat may increase production of cancer promoter lipoperoxides. On the other hand, use of iron chelation or iron mediated oxidative assault for the treatment or prevention of cancer appears to be promising; but further research is required. Considering this background, this article reviews the literature and evidence, focusing on the role of iron overload and deficiency in developing and treatment of various cancers.
Keywords
Iron Overload Deficiency Neoplasms
1. Introduction
Cancer is a global health problem and leads to more than 7 million deaths each year (1). Among all cancer cases, only 5% - 10% are caused by genetic defects and the remaining 90% - 95% are due to modifiable factors such as lifestyle factors (including smoking, diet and nutrition, alcohol, physical inactivity, obesity, sun exposure and physical activity), infections and environmental pollutants. Therefore, many cancers are preventable by altering risk factors. Within the lifestyle factors, the critical role of nutrition and related factors in incidence of cancers is universally accepted (2). Diet is estimated to account for approximately 30% of cancer deaths (3) and observational evidence suggests that altering nutritional factors and food consumption patterns may prevent about 30% - 40% of cancer cases (2). Among these nutritional factors, iron is a nutrient which is essential for many cellular processes, including energy production, oxygen transport, and DNA synthesis (4, 5).
Iron has the ability to cycle between its two forms, ferric (Fe3+) and ferrous (Fe2+) states, and consequently, has the nature of electron donor and acceptor and possesses redox activity. Therefore, it is a key cofactor for many enzymes involved in important biochemical pathways (4). Iron in hemoglobin, myoglobin, and enzymes serves as functional iron, whereas iron in ferritin, hemosiderin, and transferrin is storage iron (6). The normal serum ferritin levels in adult men and women are 12 - 300 ng/mL and 12 - 150 ng/mL respectively (7). Through breakdown of red blood cells by reticuloendothelial system, approximately 90% of iron is recovered and a small part of the iron enters into the body and is excreted daily (6, 8). States of iron overload or deficiency occur when regulatory mechanisms for extra- and intracellular iron levels do not work as expected or when the amount of iron input is outside the physiological range (9). The iron content of a diet including animal sources is roughly 6 mg/1000 kcal, consequently, the typical 2000 kcal diet of a woman in her childbearing years meets only 67% of her requirement. In contrast, the median iron consumption by men is mostly more than the RDA for them (6). Both states of iron deficiency and overload can result in adverse effects on the optimal health. It is believed that excessive iron can have a role in developing chronic diseases such as cancer, diabetes, and coronary heart disease. On the other hand, iron deficiency in addition to iron deficiency anemia may also lead to more serious consequences such as incidence or recurrence of some cancers (5, 6, 9-14). Similar to incidence and recurrence of cancer, the role of iron in the treatment of cancer has been studied in two directions. Depriving cancer cells from iron with iron chelators has been proposed as a therapeutic approach for cancer. Manipulation of iron stores in cancer cells for treatment of cancer has been considered in the other direction as well, so that iron overload in cancer cells results in inhibition of cancer growth by generating oxidative assault (15, 16). Against this background, we performed a review of the literature, focusing on the role of iron overload and deficiency in developing and treatment of various cancers. We aimed to clarify that the risk of which types of cancers may be elevated by iron deficiency and which types of cancers are in relation with more iron consumption and higher amounts of iron status indicators. In terms of iron consumption, we aimed to know whether there is a difference between the two forms of dietary iron (heme and non-heme). We also aimed to discuss the mechanisms through which iron chelation and iron containing drugs may have cancer therapeutic properties.
Related mechanisms of therapeutic and carcinogenic effects of iron overload and iron deficiency are shown in Figure 1.
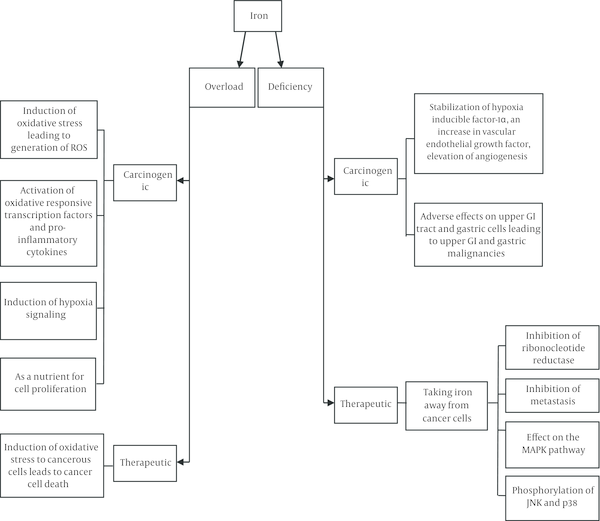
2. Carcinogenic Effects of Excess Iron
Iron overload generally occurs when total body iron exceeds 5 g (8). As taking too much iron from foods or dietary supplements may contribute to production of reactive oxygen species (ROS) (11, 17), excess accumulation and storage of iron because of food fortification and use of iron supplements may be contributing to increased risk of cancer (6, 18).
Iron-induced ROS generation is thought to originate from the interaction between iron and superoxide (O2-) (Haber-Weiss reaction) and/or hydrogen peroxide (H2O2) (Fenton reaction) (8).
Fe3+ + O2-→ Fe2+ + O2
Fe2+ + H2O2 → Fe3+ + OH- + OH
Highly reactive hydroxyl radicals generated by the reaction between iron and hydrogen peroxide are extremely damaging to biomolecules and can promote oncogene activation, DNA strand breaks, lipid peroxidation, mutagenesis and tumor suppressor inhibition (19, 20). Hydroxyls radicals increase oxidative stress and result in increased free iron concentrations by the Fenton and Haber-Weiss reactions (17). ROS which are recognized to serve as a second messenger in intracellular signaling cascades, promote and maintain the oncogenic phenotype of cancer cells (11, 21, 22). ROS-activated signal-transduction pathways include the mitogen-activated protein kinase (MAPK) pathway, the AP-1 pathway, and the nuclear factor-κB (NF-κB) pathway, which impress transcription of genes involved in transformation and cell growth (11).
2.1. Heme versus Non-Heme Iron Carcinogenicity
As mentioned before, total dietary iron is found in two forms, heme (10%) and non-heme (90%) iron (23). Major sources of heme iron are meat, pork, and fish. Foods with a high content of non-heme iron are dried beans and vegetables (6, 14).
The association between red and processed meat intake, and colorectal cancer and the potential mechanisms of these relation have been investigated in a large cohort study by Cross and others (24). For both red and processed meat intakes, there was an elevated risk of colorectal cancer (HRQ5vs. Q1, 1.24; 95% CI, 1.09 - 1.42; P trend < 0.001; HRQ5vs. Q1, 1.16; 95% CI, 1.01 - 1.32; P trend = 0.017 respectively). But intake of white meat was not associated with colorectal cancer risk. Daniel and others in a large cohort prospective study investigated the relation of poultry and fish intake, and risk of various malignancies in men and women. In substitution models, a 10 g (per 1,000 kilocalories) increase in white meat intake substituted for an equal amount of red meat intake (total meat intake held constant) was associated with 3% - 20% reduction in risk of esophagus, liver, colon, rectum, anus, lung, and pleura cancers (25). The potential carcinogenicity of red meat might be because of heat-induced mutagens, excess fat, protein, or iron, salt and nitrite in processed meat (26). The difference in the results between red and white meat is likely to be because of a compound absent in white meat (26). The iron content is one major difference between red and white meat (24), and the major cancer promoter in red meat is presumably heme iron and not the other constituents or preparation methods of meat (26, 27). In a recent case-control study, a strong relationship was observed between red meat consumption and lung cancer (OR = 2.9, 95% CI = 1.8 - 4.7) (28). Tasevska and others investigated the association between heme iron and lung carcinoma. In this prospective study, heme iron intake was positively associated with lung carcinoma in both men [HR Q5 vs. Q1: 1.25; 95% CI: 1.07 - 1.45; P for trend = 0.02] and women [HR Q5 vs. Q1: 1.18; 95% CI: 0.99 - 1.42; P for trend = 0.002] with a dose-dependent relationship (29). In other study, the promotion of experimental carcinogenesis in colon was dose-responsely associated with heme iron in diet and the number of mucin-depleted foci/colon in chicken (low heme)-, beef (medium heme)-, and blood sausage (high heme)-fed rats were 1.2 ± 0.6 (P = 0.13), 1.9 ± 1.4 (P < 0.01), and 3.0 ± 1.2 (P < 0.001) (26, 30). In contrast to heme iron, promotion of colorectal carcinogenesis with inorganic iron has not been shown in several studies (26). In a study in rats, elevated colonic epithelial proliferation and fecal water cytotoxicity were specific for equimolar dietary ferric citrate, heme and protoporphyrin did not have such effects (31). The effect of a diet overloaded with ferric citrate on incidence of aberrant crypt foci in mice has been investigated in a study where the results shown ferric citrate may play a role in tumor promotion, but is not adequate to beginning of tumor formation (26, 32). Cross and others found an increased risk for colorectal cancer among those with higher intakes of red meat (HR = 1.24, 95% CI: 1.09 - 1.42; P trend < 0.001). It was noteworthy that the risk of colorectal cancer was inversely associated with total iron intake and dietary iron (HR = 0.75, 95% CI: 0.66 - 0.86, P trend < 0.001; HR = 0.75, 95% CI: 0.65 - 0.87, P trend < 0.001, respectively), but positively associated with heme iron [Q5 vs. Q1 HR = 1.13, 95% CI: 0.99 - 1.29, P trend = 0.022] (24).
The cancer promotion effect of heme is probably via two independent pathways: the fat peroxidation pathway and the N-nitroso pathway (24, 26). N-nitroso compounds (NOCs), which are carcinogens in many organs such as bladder, stomach, esophagus, nasopharynx, and colon (33, 34), include nitrosoguanidines, nitrosamines, and nitrosamides (34, 35). Nitrate and nitrite which are precursors to NOCs are added to processed meat for preservation and improvement of color and flavor (33). These compounds contribute to endogenous and exogenous formation of NOCs (24, 33). It is estimated that 45% - 75% of the total NOC exposure results from endogenously formation of these compounds (34). Some human studies demonstrated that red but not white meat increases endogenous N-nitrosation with a dose-response manner. Increased endogenous formation of NOCs with increasing red-meat intake is presumably because of heme content of the red meat (27, 34, 35). Cross and others in a controlled study of 21 healthy male volunteers found that individuals on a high (420 g) red meat diet had significantly greater (P = 0.001) levels of fecal NOCs than those on a low (60 g) meat diet. They also demonstrated that endogenous N-nitrosation was increased by supplementation with heme iron (8 mg) (P = 0.006), but inorganic ferrous iron (35 mg) had no effect (35). On the whole, it seems that heme iron not inorganic iron causes endogenous formation of NOCs which once absorbed can induce tumors in many organs. In terms of meat intake, endogenously NOC formation with consumption of 60 g/d red meat was not more than levels formed by a diet with no meat (36). Furthermore, one of the new recommendations for cancer prevention is limiting the intake of red meat, the most important source of heme iron, to 500 g/wk (37).
Another mechanism linking heme iron and cancer is thought to be the fat peroxidation pathway (38). Lipid peroxidation results in formation of end products, such as alkanes, aldehydes [malondialdehyde (MDA) and 4-hydroxynonenal (4- HNE)], and isoprostanes [8-iso-prostaglandin-F2α (8-iso-PGF2α)] (26, 38). MDA cause DNA damage by binding to DNA and producing mutagenic adducts. 4-HNE selectively triggers apoptosis in normal cells but the precancerous cells that are mutated on the Apc gene are resistant to apoptosis induction (26). The main urinary metabolite of 4-HNE is 1,4-dihydroxynonane mercapturic acid (DHN-MA) which was used as a biomarker of colon cancer risk by Pierre and others (38) and its urinary excretion in rats was shown to be associated with carcinogenesis promotion by dietary heme iron (26). The results of human study showed high-heme intake increase DHN-MA by 2-fold (P < 0.001). However, non-heme iron had no association with DHN-MA excretion (38). Selected publications on type of dietary iron in relation to cancer are listed in Table 1.
| Measured Iron | Tumor Type | Compared Quantiles (Range or Median) | Relative Risk/Hazard Ratio/Odds Ratio (95% CI) | P for Trend | Type of Study, Years of Follow-Up | Population | References |
|---|---|---|---|---|---|---|---|
| Heme iron | Breast | H vs. l quintile (≥ 216.7 µg/1000 kcal vs. <62.9 µg/1000 kcal) | 1.01 (0.89 - 1.14) | 0.97 | Cohort 6.5 y | Postmenopausal women | (39) |
| Supplemental iron | Breast | H vs. l tertile (21.4 - 39.4 mg/d vs. 0.0) | 1.00 (0.74-1.35) | 0.94 | Cohort 5.5 y | Postmenopausal women | (40) |
| Heme iron from meat | Breast | H vs. l quintile (> 0.23 - 1.49 mg/1000 kcal vs. ≤ 0.07 mg/1000 kcal) | 1.12 (0.92 - 1.38) | 0.59 | Cohort 5.5 y | Postmenopausal women | (40) |
| Heme iron | Breast | H vs. l quintile (> 2.95 mg/d vs. < 1.58 mg/d) | 1.03 (0.90-1.18) | 0.25 | Cohort 16.4 y | Pre- and postmenopausal women | (41) |
| Animal source iron (largely heme) | Breast | H vs. l quartile (details are not mentioned) | 1.50 (1.19-1.88) | < 0.01 | Population based case-control | Pre- and postmenopausal women 3452 cases 3474 controls | (42) |
| plant source iron | Breast | H vs. l quartile (details are not mentioned) | 0.99 (0.75-1.29) | 0.88 | Population based case-control | Pre- and postmenopausal women 3452 cases 3474 controls | (42) |
| Heme iron | Endometrial | H vs. l quintile (> 2.95 mg/d vs. < 1.58 mg/d) | 0.82 (0.59 - 1.16) | 0.22 | Cohort 16.4 y | Women | (43) |
| Non-heme iron | Endometrial | H vs. l quintile (> 40.30 mg/d vs. < 14.25 mg/d) | 1.10 (0.79-1.53) | 0.50 | Cohort 16.4 y | Women | (43) |
| Heme iron | Endometrial | H vs. l quartile (1.63 - 21.13 mg/d vs. 0 - 0.69 mg/d) | 1.24 (1.01-1.53) | 0.02 | Cohort 21 y | Women | (44) |
| Heme iron | Colorectal | H vs. l quintile (> 2.95 mg/d vs. < 1.58 mg/d) | 1.06(0.80-1.42) | 0.99 | Cohort 16.4 y | Women aged 40-59 from the general Canadian population | (45) |
| Heme iron | Colorectal | H vs. l quintile ( 335.8 µg/1000 kcal 48.1 µg/1000 kcal) | 1.13 (0.99-1.29) | 0.022 | Cohort 7 y | Men and women aged 50 - 71 | (24) |
| Heme iron | Prostate | H vs. l quintile (366.8 µg/1000 kcal vs. 57.9 µg/1000 kcal) | 1.09 (1.02 - 1.17) | 0.003 | Cohort 9 y | Men aged 50-71 | (46) |
| Heme iron | Lung | H vs. l quintile (> 285.2 µg/1000 kcal vs. ≤ 90.2 µg/1000 kcal) | 1.25(1.07-1.45) | 0.02 | Cohort 8 y | Men aged 50-71 | (29) |
| Heme iron | Lung | H vs. l quintile (> 217.2 µg/1000kcal vs. ≤ 63.2 µg/1000 kcal) | 1.18(0.99-1.42) | 0.002 | Cohort 8 y | Women aged 50 - 71 | (28) |
| Heme iron | Renal cell carcinoma | H vs. l quintile (336.0 µg/1000kcal vs. 48.1 µg/1000 kcal) | 1.15 (0.94-1.40) | 0.03 | Cohort Over 9 y | Men and women aged 50 - 71 | (47) |
| Heme iron | Papillary renal cell carcinoma | H vs. l quintile (336.0 µg/1000 kcal vs. 48.1 µg/1000 kcal) | 2.36 (1.16-4.83) | 0.003 | Cohort Over 9 y | Men and women aged 50 - 71 | (47) |
2.2. Effects of Meat Processing on Iron Carcinogenicity
Most frequent treatments used for meat processing are salting, curing (adding sodium nitrite), smoking, cooking, drying and packaging (48). Santarelli and others summarized the results of three meta-analyses which estimated colorectal cancer risk in association with fresh red meat and processed meat intake. Processed meat intake was more closely associated with the risk of colorectal cancer than the consumption of fresh red meat. In the three meta-analyses one gram of processed meat is eleven-times, six-times or twice more carcinogenic than one gram of fresh red meat. The estimated excess risk of colorectal cancer was 17%, 19% and 22% for fresh red meat intake, and 49%, 31% and 20% for processed meat intake. The heme content in most processed meat products is less than that in fresh red meat (48). Thus, the difference between fresh and processed meat may be explained by the changes in heme molecule during processing. Through processing, NO from nitrite can react with heme to form nitrosyl heme, thus sodium nitrite nitrosylates the myoglobin heme in raw meat. Further cooking denatures globin, so that the pink nitrosyl heme which is speculated to be more toxic than native heme, can be released (48, 49). Santarelli and others investigated the effect of meat processing on carcinogenesis promotion. According to them, nitrosyl heme concentration in meat was modified by added nitrite (P < 0.01) and they found the highest concentrations of nitrosyl heme in oxidized high-heme cooked meat with added nitrite. Rats fed with this kind of meat compared to the other groups had much more ATNC excretion, heme in fecal water and more MDF per colon. These findings show that heme or nitrosyl heme may be responsible for the cured meat-induced promotion (49).
Heterocyclic amines (HCAs) are a group of potent mutagens and animal carcinogens found in cooked meats, particularly in well-done meats. Cooking at higher temperatures for longer periods of time leads to more HCA formation. Significant amounts of HCAs are found in fried, broiled, and barbecued meats. Reaction of creatine or creatinine, amino acids, and sugar over high-temperature preparation of meat results in generation of these compounds. Three of HCAs present in meat are 2-amino-3, 8-dimethylimidazo [4,5-f] quinoxaline (MeIQx), 2-amino-3,4,9-trimethylimidazo [4,5-f] quinoxaline (DiMeIQx), and 2-amino-1-methyl-6-phenylimidazo[4,5-b]pyridine (PhIP). Many HCAs have raised the development of breast, lung, large intestine, forestomach, and prostate malignancies in experimental studies (48, 50, 51). It has been shown that iron can increase the formation of MeIQx (8-MeIQx). This is attributable to the ability of iron to catalyze lipid oxidation which results in the formation of free radicals (52). Furthermore, nitrosation of HCAs such as 2-amino-3-methylimidazo [4,5-f] quinoline (IQ) or MeIQx generates N-nitroso compounds, which may trigger colon cancer under inflammatory conditions in individuals who consume well-done red meat diets (48, 53). Lakshmi and others have demonstrated that heme can augment the nitrosation of some HCAs. In the presence of 10 µmol hemin, nitrosation of IQ and MeIQx to 14C-2-nitrosoamino-3-methylimidazo [4,5-f] quinoline and 2-nitrosoamino-3,8-dimethylimidazo [4,5-f] quinoxaline increased 22-fold and 13- or 16-fold respectively (53, 54).
High hydrostatic pressure can be used as a food processing and preservation method that has little impact on nutrient content of foods but can affect the structure of proteins (55). Foods that contain peroxidable fatty acids and pro-oxidant substances are susceptible to lipid peroxidation (38). Polyunsaturated fatty acids in meat (and fish) treated at pressures of 400 MPa and above become more susceptible to oxidation. Lipid oxidation enhancing effect of high pressure treatment in meat was inhibited by metal chelating agents such as EDTA, suggesting that the release of iron from iron complexes such as hemosiderin and ferritin in meat is presumably responsible for the increased rate of lipid oxidation in meat (56). Greater peroxidation of fat in foods leads to formation of the lipoperoxides which are cancer promoters (48).
2.3. Epidemiologic, Animal, and Cellular Data on Iron Carcinogenicity
Selected publications on the relationship between total iron intake and various cancers are represented in Table 2.
| Measured iron | Tumor Type | Compared Quantiles (Range or Median) | Relative Risk/Hazard Ratio/Odds Ratio (95% CI) | P for Trend | Type of Study, Years of Follow Up | References |
|---|---|---|---|---|---|---|
| Total dietary irona | Colorectal | H vs. l quartile (> 10.3 mg/1000 kcal vs. ≤ 7.4 mg/1000 kcal) | 0.98 (0.62 - 1.55) | 0.98 | Nested case-control | (57) |
| Total dietary ironb | Colorectal | H vs. l quintile (≥ 14.99 mg/d vs. < 11.90 mg/d) | 1.07 (0.80 - 1.43) | 0.94 | Cohort, 16.4 y | (45) |
| Total dietary ironc | Colorectal | H vs. l quintile (36.1 mg/d vs. 10.8 mg/d) | 0.75 (0.66 - 0.86) | < 0.001 | Cohort, 7 y | (24) |
| Total dietary ironc | Pancreatic | H vs. l quintile ( 35.9 mg/d vs. 10.8 mg/d) | 0.93 (0.65 - 1.34) | 0.82 | Cohort, 20 y | (58) |
| Total dietary irona | Prostate | H vs. l quintile (37.4 mg/1000 kcal vs. 11.9 mg/1000 kcal) | 1.08 (0.94 - 1.25) | 0.24 | Cohort, 9 y | (46) |
| Total dietary ironb | Breast | H vs. l quintile (≥ 10.1 mg/1000 kcal vs. < 6.8 mg/1000 kcal) | 1.02 (0.90 - 1.15) | 0.94 | Cohort, 6.5 y | (39) |
| Total dietary ironb | Breast | H vs. l quintile (≥ 14.99 mg/d vs. < 11.90 mg/d) | 0.97 (0.85 - 1.10) | 0.63 | Cohort, 16.4 y | (41) |
| Total dietary ironc | Breast | H vs. l quintile (> 31.2 - 68.6 mg/d vs. ≤ 11.4 mg/d) | 1.08 (0.90 - 1.30) | 0.58 | Cohort, 5.5 y | (40) |
| Total dietary ironb | Breast | H vs. l quintile (>10.3 - 37.5 mg/1000 kcal vs. ≤ 6.9 mg/1000 kcal) | 1.25 (1.02 - 1.52) | 0.03 | Cohort, 5.5 y | (40) |
| Total dietary irona | Breast | H vs. l quartile (details are not mentioned) | 1.31 (0.96-1.78) | 0.10 | Population based case-control | (42) |
| Total dietary ironb | Breast | H vs. l tertile (16.8 mg/d vs. 9.0 mg/d) | 1.21 (0.65 - 2.26) | Χ2 (trend) = 0.3 | Case-control | (59) |
| Total dietary ironb | Endometrial | H vs. l quintile (≥ 14.99 mg/d vs. < 11.90 mg/d) | 0.90 (0.64-1.26) | 0.22 | Cohort, 16.4 y | (43) |
| Total dietary irona | Endometrial | H vs. l quartile (15.09 - 63.05 mg/d vs. 3.83 - 12.27 mg/d) | 1.31 (1.07-1.61) | 0.009 | Cohort, 21 y | (44) |
a Consideration of supplemental iron is not mentioned.
b Does not include supplemental iron.
c Includes supplemental iron.
2.4. Breast Cancer
Breast cancer is the most common cancer among women (60). It is noted that human breast cancer tissues may have excessive accumulation of iron (61), but epidemiologic studies have paid little attention to the potential effect of elevated body iron stores or excessive iron consumption on the development of breast cancer (19). Menopause contributes to a rise in body iron stores in women (19) and elevated concentration of iron may be a risk factor for breast cancer development, because it augments oxidative stress and maintains MAPK activity that are two main mechanisms for the occurrence of this cancer (62). Iron-induced oxidative DNA damage and lipid peroxidation contribute to carcinogenesis in breast (41). Besides being a pro-oxidant, high levels of free iron may reinforce the effects of ethanol and exogenous estrogens in breast carcinogenesis via accelerated production of ROS (19, 41, 63).
Two cohort studies by Kabat and others revealed no relationship between iron or heme iron and breast cancer risk. Using data from Canadian national breast screening study and national institutes of health-AARP (NIH-AARP) diet and health study, no relation between iron, heme iron or iron from meat consumption and risk of breast cancer was observed (39, 41). Moreover, in the subgroups of alcohol consumption and taking hormone replacement therapy no association between iron or heme iron intake with breast cancer risk was observed, which suggests that the effect of alcohol or estrogen is not modified by iron (39, 41), while in a cohort study by Lee and others in high alcohol drinkers a positive relation between both dietary iron and heme iron and risk of breast cancer was found (64). In one study, it was seen that consumption of non-heme iron and risk of breast cancer were not associated with each other (41); however, use of iron supplements which contribute to non-heme and total iron intake was failed to be considered (41, 43). Consistent with the data of Kabat and others (39, 41), in the case control study by Adzersen and others (65) no significant association between iron intake and risk of breast cancer was found. Null results of some studies which investigated the association between iron intake and breast cancer may be a result of low participation of iron intake in making iron stores in the body, as intestinal iron uptake contributes to only < 0.05% of iron reserves in the body (66). Moreover, dietary antioxidants may modify the role of free iron in oxidative stress (39). In a prospective study data of 1205 postmenopausal breast cancer cases were interpreted and a positive association was seen for dietary iron (HR: 1.25; 95% CI: 1.02, 1.52; P trend = 0.03) and red meat (HR: 1.23; 95% CI: 1.00 - 1.51, P trend = 0.22) with the risk of breast cancer, but the investigators did not observe any associations for meat iron, heme iron and iron from supplements (40). A population-based case-control study by Kallianpur and others revealed a positive association between animal-derived (largely heme) iron intake and breast cancer risk (P trend < 0.01; OR = 1.49, 95% CI: 1.25 - 1.78). Moreover, iron and fat from animal sources had a significant interaction (P < 0.01), which means that animal-derived saturated and mono-unsaturated fats may have a strengthening effect on the role of animal-derived iron in breast cancer (42).
Individual’s genetic profile and specifically, polymorphisms which are related to iron-induced oxidative stress, are likely to have a modifying effect on the role of iron in breast carcinogenesis (67). Hong and others in a nested case-control study of postmenopausal women, assessed whether polymorphisms in genes working in the production and elimination of iron-related ROSs (i.e., Nrf2, NQ01, NOS3, and HO-1) are related with risk of breast cancer. They found a significant dose trend (P trend = 0.04) for overall number of at-risk alleles (Nrf T, NQO1 T, NOS T, HO-1 LL, and LM genotypes) so that in comparison with women who did not have any at-risk alleles. Furthermore, genetic profiles, iron consumption, and risk of breast cancer had a significant interaction with each other. In the third tertile of overall iron consumption (dietary plus supplemental) which meant consuming > 22.5 - 98.2 mg/d total iron, possessing three high-risk alleles or more was the high-risk genotype and brought about an OR of 2.27 [95% CI: 0.97 - 5.29 (P for trend = 0.02)] compared to those without any high-risk alleles. An OR of 2.39 [95% CI: 1.09-5.26 (P for trend = 0.02)] was observed for women who consumed multivitamin supplements containing iron and possessed the high-risk genotype as well (67). Nineteen sequence variations at TFR1, TFR2, HFE, and FPN1 were examined by Abraham and others and genotype frequencies were studied among 688 cases and 724 controls for realizing whether there is a relation between mutations in hemochromatosis and transferrin receptor system and breast cancer. Genotype and allele frequencies did not indicate to be significantly different among the two groups, but the incidence of the HFE Tyr282 minor allele in patients with breast cancer who had four or more involved lymph nodes was 2.6-fold higher (P = 0.032) (61). Kallianpur and others (68) concluded that HFE Tyr282 allele was more frequent in a group of cases with breast cancer from Tennessee in comparison with women from the same state or the general population (P < 0.001). These observations may be explained by the elevated cellular iron uptake associated with the HFE Tyr282 allele (69) or the high iron content in breast cancer cells (61). However, these observations are limited to a low number of patients (61, 68).
Increased iron reserves due to decreasing menstrual periods, when a woman is getting menopause, might significantly affect the breast carcinogenesis in women (11, 12, 70). High levels of iron increase oxidative stress and activate mitogen-activated protein kinase (MAPK), which may participate in breast cancer development (11, 62). Furthermore, cessation of ovarian functions leads to decreased estrogen level (12). Jian and others examined the effect of iron accumulation on menopause-related breast cancer using cell culture models which had low estrogen and high iron level. The results showed that MCF-7 cells grown in postmenopausal conditions of low 17ß-estradiol (E2) and high Fe were oxidatively damaged as determined by lipid peroxidation. In the presence of H2O2 (10 µM H2O2 for 4 hours), MCF-7 cells grown in postmenopausal conditions derived significantly lipid peroxidation, but the same cells grown in premenopausal conditions were supported from H2O2-induced lipid peroxidation (62).
2.5. Colorectal Cancer
The initiation or promotion of colorectal cancer, the third common malignancy in the world, might be linked to the existence of elevated concentration of iron in the fecal stream and its subsequent formation of free radicals (8, 71, 72). Large prospective epidemiological studies have examined the association between iron from exogenous (dietary) or endogenous (body store) sources and colorectal cancer (CRC) risk (8, 73, 74). A recent meta-analysis of prospective studies found a significant positive dose-response relationship between heme iron intake and CRC risk (75).
A paper published in 1999 examined the effect of intraluminal iron obtained from diet or oral supplementation on free radical production in feces and demonstrated that free radical formation intensifies during iron supplementation and that taking ferrous sulfate in healthy volunteers increases fecal concentration of iron with the ability of forming free radicals (71). Therefore, it was assumed that orally taken iron which fails to be absorbed and reaches the colon may damage mucosa by intensifying formation of free radicals to a critical level (71, 76). Impact of prolonged intake of iron on mucosal lipid peroxidation and production of free radicals in the colon and cecum was analyzed in male Wistar rats by Lund and others and demonstrated to be able to elevate the both measured variables in large intestine and cecum (77).
Intake of iron, more specifically heme iron from meat, is one of the explanations for the association between meat consumption and risk of colon cancer besides the presence of heterocyclic aromatic amines in well-done fried meat, the endogenous formation of carcinogenic N-nitroso compounds (which is also related to heme iron intake) and dietary fat (31, 57, 78, 79). On the other hand, the difference of red and white meat in promoting colon malignancy is probably explained by the fact that there are higher amounts of heme in red meat in comparison with white meat (31). According to the recent population-based cohort study in Japan, exposure to dietary heme iron was not significantly related to development of colorectal adenoma (57, 80). Bastide and others conducted an analysis of investigations in rats in which colon malignancy was developed by chemical substances. They concluded that red meat and food derived hemoglobin increase abnormal crypt foci (79). In a study by Sesink and others large intestinal epithelial proliferation was elevated in heme-fed rats, in which the degree of cytotoxicity of fecal water was higher than the control group. However, heme-induced cytotoxicity did not seem to be merely resulted from the activity of reactive oxygen species because the cytotoxicity of fecal water did not vary between anaerobic and aerobic situations. Therefore, this may imply that an unidentified factor which is toxic to cells may be produced in the large intestinal lumen as a result of dietary heme metabolism (8, 31).
A study of 49,654 Canadian women (45, 81) and a follow-up study by Zhang and others (81) found no association of dietary iron intake, heme iron,iron from meat, total iron intake, and iron supplement use with risk of colorectal cancer, and alcohol consumption or use of hormone therapy did not affect these results significantly. In a recent population-based case-control study although no association between intake of dietary iron and malignant neoplastic disease of colorectum was demonstrated in men, an inverse relation was observed in women (OR = 0.45; 95% CI = 0.22 - 0.92). Iron supplementation had a direct association with the incidence of colorectal cancer in both sexes, so that use of 18 mg/d supplemental iron compared to 0.0 mg/d showed an OR of 2.31 (95% CI = 1.48 - 3.59; P trend < 0.001) (82). Both Bird and others (10) and Cross and others (57) suggested that iron may be involved in the early phases of colorectal carcinogenesis and that the risk of developing colorectal polyps or adenoma may decline, if iron reserves in the body are lower. Excepting subjects whose ferritin levels may represent inflammation or aging rather than iron stores, there was a significant positive relation between ferritin and colorectal polyps as an intermediate marker for colorectal cancer. Moreover, this ferritin-polyps relation was supported by the relation between polyps and iron intake, so that in comparison with those who consumed iron adequately (11.6 - 13.6 mg/d), those whose iron intake was > 27.3 mg/d had a multivariate-adjusted OR of 1.4 (95% Cl 0.9 - 2.0) (10). Similarly, higher serum total iron binding capacity (TIBC) and unsaturated iron binding capacity which indicate lower iron status in the body were associated to lower risk of developing colorectal adenoma (57). Wurzelmann and others in 1996 reported that subjects with colorectal cancer had higher transferrin saturation (30.7% vs. 28.7%, P = 0.05) and serum concentration of iron (107.7 vs. 100.4 µg/dL, P = 0.03) in comparison with individuals without the disease (83). Chan and others despite measurement of a variety of parameters which affect iron exposure (i.e., biomarkers including transferrin saturation and the ratio of the concentrations of soluble transferrin receptors to ferritin, genetic mutations, and dietary consumption) did not support involvement of iron or the HFE genotype in the mechanisms through which colorectal neoplasia develops in women (84). Selected publications on the association between iron status and risk of different cancers are listed in Table 3.
| Measured iron | Type of Tumor | Comparison of Quantity of Intakes | Relative Risk/ Odds Ratio (95% CI) | p for Trend | Type of Study | Population, Number of Cases | References |
|---|---|---|---|---|---|---|---|
| Ferritin (ng/ml) | Colorectal | H vs. l quartile (>276 vs. ≤ 83) | OR = 0.86 (0.53 - 1.38) | 0.08 | Nested case-control | Men and women aged 58 - 66 y, 356 cases 396 controls | (57) |
| TIBC (µg/100 ml) | Colorectal | H vs. l quartile (> 389 vs. ≤ 323) | OR = 0.57 (0.37-0.88) | 0.03 | Nested case-control | Men and women aged 58-66 y, 356 cases 396 controls | (57) |
| Transferrin saturation% | Colorectal | > 60% vs. ≤ 60% | RR = 3.04 (1.64 - 5.62) | - | Cohort | Men and women, 173 | (85) |
| Ferritin (µg/L) | Prostate | (mean ± SEM) in cases vs. controls 156±24 vs. 245±21 | 95% CI in cases vs. controls (109 - 203) VS. (205 - 286) | P value = 0.043 | Case-control | Men aged 49 - 78, 34 cases 84 controls | (86) |
| TIBC (µmol/L) | Prostate | (mean ± SEM) in cases vs. controls 69.87±2.67 vs. 60.43±2.27 | P value = 0.0178 | Case-control | Men aged 49 - 78, 34 cases 84 controls | (86) | |
| Ferritin (µg/L) | All types of cancers | H vs. l quartile (> 160 vs. < 30) | RR = 1.88 (1.05 - 3.35) | 0.07 | Cohort | Women, 6974 female subjects (319 cancer cases) | (87) |
| Ferritin (µg/L) | Colorectal | quartile 4 vs. quartile 2 (289 - 500 vs. 73 - 141) | OR = 1.5 (1.0 - 2.3) | Case-control | Men and women aged 50 - 75, 395 cases 420 controls | (10) | |
| Ferritin (ng/mL) | Gastric | H vs. l tertile (≥ 6.0 vs. < 5.4) | OR = 0.2 (0.1 - 0.8) | 0.02 | Nested case-control | American men of Japanese ancestry, 46 cases46 controls | (88) |
| Iron (µg/100 mL) | Gastric | H vs. l quartile (> 138 vs. ≤ 88) | RR = 0.60 | < 0.01 | Cohort | Men aged 20 - 74, 120 | (85) |
| TIBC (µg/100 mL) | Gastric | H vs. l quartile (> 369 vs. ≤ 308) | RR = 1.29 | < 0.05 | Cohort | Men aged 20 - 74, 120 | (85) |
| TIBC (µg/100 mL) | Lung | H vs. l quartile (> 369 vs. ≤ 308) | RR = 0.69 | < 0.001 | Cohort | Men aged 20 - 74, 416 | (85) |
The risk of colorectal cancer has been shown to be higher in patients with hereditary hemochromatosis (HH) which results from HFE mutations (89, 90). Stevens and others in 2003 examined the impact of iron from food on MDA level in the large intestine of HFE-knockout mice to detect interactive association between iron exposure and HFE genotype in inducing oxidative damage. They found a higher large intestinal level of MDA in standard iron diet-fed mice in comparison with low iron diet fed-mice, implying that dietary iron might be able to potentiate the effect of HFE mutation on colonic oxidative damage (89). Nelson and others in 1995 showed an increased risk for colonic adenoma in HH heterozygote men (RR, 1.24; CI, 1.05 - 1.46) and women (RR, 1.29; CI, 1.08 - 1.53), and a higher risk of colorectal malignant neoplastic disease in HH heterozygote men (RR, 1.28; CI, 1.07 - 1.53) (91). Two other studies did not report a role for HFE genotypes in modifying the risk of colorectal malignancy (84, 92), but mutations in the HFE gene were related with increase in some parameters of evaluating iron reserves in the body (84).
There is evidence that the relationship between iron and colorectal cancer may differ among subsites and may be attributable to whether exposure is humoral or luminal (83). Dietary Iron intake (and particularly heme iron intake) may elevate the risk of proximal colorectal adenomas or malignancies (73, 83, 93, 94), while serum concentration of iron may elevate the risk distally (83).
2.6. Pancreatic Cancer
Excess iron has been indicated to be related to the risk of insulin resistance and type 2 diabetes. This hypothesis was suggested because type 2 diabetes is one of the most seen complications of HH (95, 96). The association between higher levels of iron reserves as measured by serum ferritin levels and type 2 diabetes has been shown in some prospective studies (97, 98). On the other hand, there is evidence that strongly supports the relation between diabetes and elevated risk of developing pancreatic malignancy. A meta-analysis of 35 prospective studies concluded that both diabetic men and women may have an elevated risk of pancreatic cancer (99). Therefore, diabetes risk factors, including iron overload, may directly associate with pancreatic malignancy (100). Excessive accumulation of iron in the liver may bring about impairment as a result of oxidative stress and lead to insulin inefficiency in reducing glucose formation in this organ. Accumulation of iron in pancreatic β-cells may cause failure of these cells and impair insulin secretion. Therefore, iron overload may cause insulin resistance and reduction of insulin release (100, 101). The mechanism underlying the link between diabetes and pancreatic cancer might be hyperglycemia-induced oxidative stress, which stimulates precarcinogens and promotes development of neoplasm cells. Moreover, increased bioavailability of insulin-like growth factor1 may play a role in this association (58, 100). Some prospective studies have found a positive association between heme-iron intake and diabetes (102-104), but the amounts of total iron or dietary iron consumption were not shown to have any relation with diabetes (104). This difference might be due to higher bioavailibility of heme iron compared to other forms of iron (100). Some case-control (105-110) and prospective (58, 111, 112) studies have examined the association between dietary iron and pancreatic cancer risk, all of which found no association between iron intake and risk of pancreatic cancer. In a recent large cohort study neither total iron nor heme-iron was associated with risk of pancreatic malignancy. However, heme-iron intake was associated to increased risk of pancreatic cancer in female smokers (HR per 1 mg/d increase = 1.38, 95% CI = 1.10 - 1.74), and in abdominally obese men and women the relation between heme-iron intake and pancreatic cancer risk turned positive in the 5th quintile of heme-iron intake (HR = 1.89, 95% CI = 1.02 - 3.50, and HR = 2.28, 95% CI = 1.31 - 3.97, respectively). The positive association seen between each 1 mg increase in heme-iron consumption from red meat with risk of pancreatic cancer in women (HR = 1.25, 95% CI = 0.97 - 1.62), was more significant if their BMI was ≥ 25 kg/m2 or if they were smokers (100). These modifications by BMI and smoking habit could be explained by the effect of obesity on insulin resistance, increasing oxidative stress and inducing inflammation, and the impact of NOCs and other similar carcinogens between tobacco and meat (100). Furthermore, smoking habit and body weight themselves may anticipate developing pancreatic cancer (113). A case-control study with 450 pancreatic cancer patients reported that higher serum iron was associated with pancreatic cancer risk (113).
2.7. Liver Cancer
Iron overload contribute significantly as a risk factor of hepatic carcinogenesis (114). HH is a primary iron-related abnormality (115) and a human disease in which excessive iron accumulation in the liver occurs due to inappropriate high absorption of dietary iron (116). Hepatic iron overload in HH often damages hepatocytes, stimulates hepatic stellate cells and increases formation of extracellular matrix components (116). Thus, it often causes fibrosis and cirrhosis and might lead to the development of hepatocellular carcinoma (HCC) (116, 117). The prevalence of HCC in HH patients is 200-fold higher than the general population (118). Oxidative stress which occurred by iron overload is the key mechanism of iron carcinogenesis (20). Oxidative stress contributes to peroxidation of unsaturated fatty acids and subsequently generation of by-products of this reaction that disrupts cell activities and protein synthesis and causes damage to DNA (117). HCC is seldom seen in patients without cirrhosis (119). A significant positive relation between higher serum ferritin concentrations and risk of primary hepatocellular carcinoma was observed in chronic hepatic patients from Korea (120). However, in more than half of non-cirrhotic patients who develop HCC a mild iron overload could be diagnosed (8). Therefore, the view of cirrhosis, not the iron overload being the cause of hepatocellular malignancy may not be true (117). In a cohort study of 5224 individuals having liver transplantation, there was a significant relation between any excessive accumulation of iron and HCC (P = 0.001), and the association stayed significant even after adjustment for the cause of liver disease (121). In three case-control studies African iron overload was shown to be a risk factor in the pathogenesis of HCC (122-124). Iron overload in Africa occurs as a result of consuming a traditional fermented beverage with high iron content; thus, it has been perceived as having an environmental etiology (125). However, an interaction between the iron intake from diet and a non-HLA-linked iron loading gen may contribute toward the pathogenesis of dietary iron overload (126). In an experimental study on long-evans cinnamon (LEC) rats which have been found to store abnormally high amount of iron in the liver, Kato and others in 1996 compared developing hepatitis and liver cancers in LEC rats given an iron-deficient diet (ID) with the occurrence of these diseases in rats given a regular diet (RD) (127). They demonstrated that excessively stored iron in the liver of LEC rats was involved in the occurrence of fulminant hepatitis and hepatic malignancy. On the other hand, excessive iron accumulation in tissues and cells makes pathogens such as hepatitis B virus cause illness more easily (128), and infection with hepatitis B and C viruses are important environmental risk factors for HCC in different populations (117, 129).
2.8. Prostate Cancer
Prostate cancer is the most widespread cancer in men (130). Red meat intake has been shown to be associated with the risk of prostate cancer (131). One of the mechanisms through which meat may elevate the risk of prostate cancer is heme iron. Heme iron can increase endogenous production of NOCs, and can also cause oxidative cell damage through free radical formation (46, 132).
Human prostate tissues are susceptible to oxidative damage to DNA (133), and heme induced oxidations can cause damage to DNA and other nucleic acids which is comparable to the damage caused by ionizing radiation (134). Intracellular ROI formation and activation of NF-κB-mediated signaling pathways by iron trigger uPA production in the human prostate cancer cell line, PC-3. Higher expression of tumor-associated uPA in prostate cancer-suffering men contributes to elevated spread of tumor and poor consequences of cancer (135). The results of a systematic review suggested that excessive meat consumption may associate to increased risk of prostate cancer (136). Among participants in the NIH-AARP cohort a 9% higher risk for overall prostate malignant disease (HR = 1.09 (95% CI: 1.02, 1.17) and a 28% higher risk for advanced disease (HR = 1.28 (95% CI: 1.03, 1.58) were seen in relation to heme iron intake (46). In a review of meat intake in relation to prostate cancer 9 of 27 case-control and cohort reviewed studies showed a statistically significant positive risk with higher total meat intake (137). Alexander and others in 2010 conducted a meta-analysis of prospective studies about the association of red and processed meat intake and risk of prostate cancer. Total prostate malignant neoplastic disease had no relevance with each 100 g increase in red meat (SRRE = 1.00, 95% CI: 0.95 - 1.05) or with high vs. low intake of red meat (SRRE = 1.00, 95% CI: 0.96 - 1.05). Similarly, advanced prostate malignancy had no relation with red meat intake (SRRE = 1.01, 95% CI: 0.94 - 1.09) (138). One possible explanation of these null findings may be the high levels of selenium and zinc in red meat (the most important source of heme iron) (132).
Foods containing antioxidants, such as selenium and zinc, which are essential for testosterone synthesis, are probably protective against prostate cancer (46, 86, 132, 138, 139). On the other hand, high consumption of foods containing lycopene may reduce risk of prostate cancer (138). Matos and others using iron for causing in vivo oxidative stress damage in rat prostate, demonstrated that lycopene and ß-carotene might suppress iron-induced oxidative DNA damage in rat prostate (140). There is inconsistent information on iron status and risk of prostate cancer. In two cohort studies, no significant differences in TIBC, serum iron levels, and transferrin saturation were observed between men who developed prostate cancer and those who did not (85, 141). Conversely, Kuvibidila and others even after taking the inflammatory status into consideration observed lower concentrations of serum ferritin and transferrin saturation and higher TIBC in men with prostate cancer compared to those without the disease. Since urinary blood loss is not common in men with prostate cancer, reduced serum ferritin and transferrin saturation in prostate cancer patients may be due to reduction of iron absorption because of inflammation and/or elevated iron utilization by prostate cancer cells (86, 142).
3. Therapeutic Effects of Excess Iron
Oxidative stress is not always damaging (143), because high levels of ROS may function as a double-edged sword (144). Moderate increase of ROS could result in proliferation and differentiation. However, the antioxidant capacity of the cell could be broken through by critically high concentration of ROS. This leads to apoptotic or necrotic cell death, depending on the degree of oxidative damage (144). On the other hand, more specifically for tumor cells, anti cancer agents would be more effective in cancer treatment (145). Based on this background, selective oxidative stress by increased reactive oxygen species or inhibition of endogenous antioxidant defense can be used as a therapeutic approach in cancerous tissues, as well as sparing normal tissues from damage (143). Improvement of this therapeutic strategy relates to understanding the biological difference between malignant and normal cells. Cancer cells are more vulnerable to oxidative assault than normal cells due to very few levels of antioxidative enzymes, such as superoxide dismutase, catalase, also glutathione peroxidase, (146-148). This lack of a proper antioxidant defense makes cancer cells more likely to be defenseless against oxidative stress induced by exogenous agents (144). Furthermore, iron metabolism in cancer cells differs from normal cells, suggesting that an iron-mediated ROS generation could be the source of oxidative assault that selectively affects malignant cells while leaving normal cells unharmed. Cancerous cells require more iron, are abler to store iron, and less able to expel it (16). The iron containing ferric-sorbitol-citrate complex was shown to suppress proliferation of cultured mouse melanoma B16, GHC, KB, HeLa and CaCo2 cells, but had no impact on the proliferation of the nonmalignant fibroblast L929 line, human bone marrow-HBS, VERO and HEF cell line. Moreover, synthesized iron substances (ferrocene analogs) had growth preventive impact on malignant mouse melanoma F10 cell lines, whereas they did not influence the viability of nonmalignant fibroblasts (149). Kiessling and others using murine T-cell lymphoma model, reported that NF-κB inhibition by specific inhibitors results in down-regulation of ferritin heavy chain (FHC) and consequently disruption in the balance of iron stores and elevation of free intracellular iron which leads to extensive formation of ROS via the fenton reaction. This finally decelerates in vivo tumor growth while normal cells remain unharmed (150). In a leading opinion paper Foy and Labhasetwar proposed that iron-oxide nanoparticles might be able to suppress tumor growth by inducing an oxidative attack against cancer without hypersensitivities associated with the dextran-complexes. They found that in athymic nude mice bearing MCF-7 xenograft tumors, treatment with iron-oxide nanoparticles effectively diminished tumor size and increased survival. They also observed that the magnetic nanoparticle formulation was non-toxic in vitro but toxic to malignant cells in vivo (16). In human breast cancer cells iron oxide nanoparticles induced substantial apoptosis, caspase-3 activity, depletion of superoxide dismutase, glutathione, and catalase activities, increased generation of reactive oxygen species, and lipid peroxidation (151).
4. Therapeutic Effects of Iron Defficiency
Iron is a fundamental nutrient to cell growth and metabolism, and is a key component of the active site of ribonucleotide reductase (RR), the rate-limiting enzyme in DNA synthesis (15). More iron requirements of cancer cells make these cells more susceptible to iron depletion in comparison with normal cells. Therefore, depriving cancer cells of this vital nutrient could be an effective strategy in the treatment of cancer (152). Iron deprivation can be induced by iron chelators which play a role in the prevention and treatment of cancer in animal models and in patients (153). Although iron depletion and the subsequent inhibition of RR were traditionally considered as the mechanisms of the growth inhibitory effects of iron chelators, recent evidence suggests the involvement of many other genes, molecules and signaling pathways (154). Moreover, iron chelators could act as chemo-preventive agents by inhibiting participation of iron in the Fenton reaction and other oxidative stress pathways induced by iron (155).
A large variety of iron chelators have been designed and further investigation is being conducted to increase their efficiency. Siderophores including Desferrioxamine, Desferrithiocin and Desferri-exochelin are low molecular weight ligands developed to sequester iron in a soluble form. In contrast to Siderophores, which are natural iron chelators, many chelators have been artificially synthesized for achieving maximum antiproliferative function or iron removal. Synthetic iron chelators consist of ICL670A, Deferiprone and hydroxypyridinone analogs (4). Tachpyridine and its analogs form another group of iron chelators that demonstrate to be a potential selective strategy for anticancer treatment. Di-2-pyridylketone thiosemicarbazone (DpT) and 2-benzoylpyridine thiosemicarbazone (BpT) which have a high affinity for iron are novel chelators which show noticeable and selective antineoplastic properties against a broad range of neoplasms both in vivo and in vitro (4, 15). Plant-derived iron chelators such as silybin and curcumin have also been shown to be effective in treating cancer (15).
Curcumin is a polyphenolic bioactive compound, extracted from the rhizome of Curcuma longa,which has been reported to have antioxidant and antiproliferative activities in human breast tumor cells and inhibitory effects on skin, oral, intestinal and colon carcinogenesis in mice (156, 157). It has been used to treat inflammatory disorders (156) and cancer (158). Curcumin possesses preventive effect on tumor growth and induces tumor cell apoptosis in animal and cell culture models and the mechanism of its cancer chemopreventive activity is multifactorial. Curcumin suppresses activation of NF-κB and COX2, changes AP1 complexes, inhibits Akt, stimulates cytoprotective phase II enzymes including glutamate-cysteine ligase, isoforms of glutathione S-transferase, heme oxygenase and NAD(P)H quinone oxidoreductase1. Furthermore, curcumin is an antioxidant and free radical remover (155) and demonstrates iron chelation properties in vitro, particularly for Fe3+ (153, 155, 158) which may lead to curcumin’s antioxidant and antiproliferative activities. In an experimental study curcumin was protective towards nigral dopaminergic neurons against 6-hydroxydopamine, which could be attributed to its iron-chelating properties (159).
Silybin, which is the main active compound of the milk thistle, has anticancer activities in a variety of epithelial cancers and possess iron chelating activity (160, 161). In an experimental study, the severity of prostatic lesions in silibinin-fed mice was less than that of positive controls (162), and in the study by Kauntz and others the number of azoxymethane (AOM)-promoted hyperproliferative crypts and aberrant crypt foci in the colon of Silibinin-treated rats were twice less than AOM-injected control rats receiving the vehicle (161). A published study reported that a 12-week treatment with a standardized silybin and soy phosphatidylcholine complex reduced body iron stores in patients with chronic hepatitis C that was attributed to the iron-chelating properties of silybin (163). Moreover, in HH patients, intake of silybin together with a meal decreased the postprandial elevation of serum iron in comparison with tea (P < 0.05) and water (P < 0.05), suggesting that silybin could be a complementary treatment for hemochromatosis (160). Silybin may also be protective against photocarcinogenesis in mice (164). This could be due to its iron chelating properties as excessive amount of iron has been demonstrated to augment promotion of chemically induced cutaneous tumor in animals (165).
There is some evidence suggesting that reducing body iron stores by blood donation may reduce the risk of cancer (166, 167). Edgren and others conducted a nested case-control study within a large cohort of Scandinavian blood donors to test the effect of reduced iron stores on the incidence of cancer. It was demonstrated that men with the largest loss of iron (> 2.7 g) with a latency of 3 - 7 years were 30% less likely to develop pulmonary, hepatic, esophageal, gastric, and colon cancers compared to those with the smallest loss of iron (< 0.75 g) during the same period of time (combined odds ratio [OR] = 0.70, 95% confidence interval [CI] = 0.58 to 0.84). The authors suggested that lack of risk reducing effect of blood donation-related iron loss among women was due to regular loss of iron through menstrual blood and less important effect of the loss through donated blood (168). In a randomized clinical trial in patients with peripheral arterial disease with no history of malignancy during the past 5 years before the entry, it was noted that iron loss caused 37% lower overall incidence of cancer. Moreover, cancer specific and all-cause mortality was reduced in those who developed cancer in the phlebotomy arm in comparison with patients in the control arm. The mean ferritin concentration among those in the phlebotomy group who developed cancer was significantly higher than those in the same group without cancer (76.4 ng/mL, 95% CI = 71.4 to 81.4 ng/mL, vs 127.1 ng/mL, 95% CI = 71.2 to 183.0 ng/mL; P = .017) (166).
5. Carcinogenic Effects of Iron Deficiency
Iron deficiency is the most common nutritional disorder worldwide, and the only significantly frequent nutrient insufficiency in developed countries (169). It is estimated that 1 to 2 billion people suffer from the deficiency of this micronutrient (170). Iron deficiency in addition to anemia may also lead to more serious consequences. Some animal experiments and descriptive observations in humans have recommended that iron deficiency may associate to increasing the risk of some cancers (10). Iron deficiency can impair antioxidant defenses and cause an elevation in oxidative stress. This insufficiency results in imbalanced mitochondrial enzymes in which iron is an important part including cytochrome C oxidase. This enzyme is crucial to oxidative metabolism and apoptotic cascade (171). Iron deficiency seems to impair cell-mediated immunity, presumably because of a decline in RR activity in the iron-deficient environment (172). Moreover, iron deficiency impairs natural killer (NK) cells cytotoxicity, maybe by decreasing the availability of interferon gamma to them that may result in an increased susceptibility to tumor development (173-175). NK cells normally recognize tumor cells and kill them by cytotoxic activity. The anti-tumor activity of NK cells is stimulated by interferon gamma (174, 176).
Plummer-Vinson syndrome (PVS) which is characterized by iron deficiency anemia, upper esophageal stricture, cervical dysphasia, and glossitis (177), seems to be associated with elevated risk of upper gastrointestinal tract carcinogenesis like gastric and esophageal carcinoma-one of the most common gastrointestinal cancers (178, 179). This association may be due to negative impacts of iron deficiency on these rapidly proliferating cells (177). There is also some information suggesting a relation between iron deficiency and gastric cancer which is attributable to premalignant lesions like chronic atrophic gastritis caused by chronic iron deficiency (180, 181). Therefore, PVS role in gastric carcinogenesis may be because of iron deficiency effects on gastric mucosa (179). Moreover, prolonged blood loss through premalignant lesions contributes to chronic iron deficiency which may cause alterations in the gastrointestinal tract and absorption of iron and other nutrients (181). In a cohort of 41,276 men and women with a mean follow-up of 14 years, for the risk of gastric cancer, Knekt and others found inverse associations with transferrin saturation and serum iron, and a positive association with TIBC (85). Nomura and others in 1992 concluded that the inverse relationship between serum ferritin and gastric cancer was probably not a direct one, with the achlorhydria occurring before the diminished serum ferritin concentrations and the diagnosis of gastric cancer (88). Noto and others in 2013 attempted to find the impact of iron deficiency on Helicobacter pylori infection pathogenicity in gastric carcinogenesis and demonstrated that iron deficiency induces Helicobacter pylori-induced carcinogenesis in rodents and humans (47). Inadequate intake of iron has also been shown to be associated with an elevated risk of oral cavity cancer. In a hospital-based, case-control study low serum concentrations of iron indicators (serum iron, transferrin saturation, and TIBC) were associated with higher risk of oral cancer except for ferritin levels. The authors suggested that it was because of ferritin being a positive responder to inflammatory conditions and chronic diseases (182).
Huang proposed that premenopausal women may be more vulnerable to return of breast cancer because of iron deficiency caused by menstruation (11). Iron deficiency results in fewer oxygen transports and consequently induces hypoxic cascade and hypoxia inducible factor-1α (HIF-1α) stabilization, which are hall markers of breast cancer malignancy and aggressiveness. HIF-1α activation leads to increased VEGF production, angiogenesis, metastasis, and consequently higher tumor grades and greater recurrence rates (11, 62, 183, 184). Jian and others in 2011 examined this assumption in cell culture models with the high estrogen and low iron levels which is similar to those in premenopausal women, and also in iron deficient diet-fed mice. The findings of this study implied that in premenopausal women with low iron status there is a pro-angiogenic situation which could result in the high recurrence of breast cancer. They also found that an elevated VEGF level in young women is presumably caused by iron deficiency and anemia instead of high estrogen concentrations (62).
6. Conclusion
Although data from current evidence on the carcinogenic role of iron deficiency and over sufficiency is mixed, there is overall support for these possibilities. Chronic iron deficiency in addition to iron deficiency anemia may increase the risk of gastric and upper gastrointestinal tract cancers. It is absolutely vital to ensure that children, women of childbearing age, and other groups at-risk for iron deficiency are taking this nutrient sufficiently. It seems that women of childbearing age do not receive adequate amount of dietary iron, the median iron consumption by men is mostly more than the RDA for them. Iron over sufficiency might be associated with the incidence of colorectal, liver, breast, and lung cancers. Studies which investigated the relationship between prostate cancer and iron produced inconsistent results. As iron intake, particularly heme iron, may be positively associated with prostate cancer while biological markers of iron status showed an inverse association with the disease. Heme iron is more likely to play a role in cancer promotion than non-heme iron as it is more efficiently absorbed (10% - 20% vs. 1% - 6%) and may also contribute to increase in nitrosation of some HCAs in well-done meats, endogenous generation of NOCs, and end products of lipid peroxidation. Furthermore, processing of meat causes some alterations in heme molecule and release of iron or nitrosyl heme from iron complexes in meat which may result in more carcinogenic effects of cured meat compared to fresh meat. Plant-based sources of (non-heme) iron have antioxidants and inhibitors of endogenous nitrosation and may modify the carcinogenic effects of iron. Moreover, an individual’s genetic profile may play a role in the iron-cancer relationship. In conclusion, to avoid adverse consequences of either iron deficiency or oversufficiency meeting body’s iron needs (8 mg/d for men and postmenopausal women, 18 mg/d for women of childbearing age) by consuming plant-based sources and white meats, avoiding processed meats and as the French National Cancer Institute recommends, limiting the intake of red meat as the most important source of heme iron to 500 g/wk are of particular importance.
Acknowledgements
Footnotes
References
Davoodi SH, Malek-Shahabi T, Malekshahi-Moghadam A, Shahbazi R, Esmaeili S. Obesity as an important risk factor for certain types of cancer. Iran J Cancer Prev. 2013; 6(4) : 186 -94
Davoodi H, Esmaeili S, Mortazavian AM. Effects of milk and milk products consumption on cancer: A review. Compr Rev Food Sci Food Saf. 2013; 12(3) : 249 -64
Beliveau R, Gingras D. Role of nutrition in preventing cancer. Can Fam Physician. 2007; 53(11) : 1905 -11
Kalinowski DS, Richardson DR. The evolution of iron chelators for the treatment of iron overload disease and cancer. Pharmacol Rev. 2005; 57(4) : 547 -83
Mascitelli L, Goldstein MR. Inhibition of iron absorption by polyphenols as an anti-cancer mechanism. QJM. 2011; 104(5) : 459 -61
Gallagher ML. Intake: The nutrients and their metabolism; mahan lk, escott-stump s, raymond jl; krause's food and the nutrition care process. 2012;
Ferritin blood test.
Huang X. Iron overload and its association with cancer risk in humans: evidence for iron as a carcinogenic metal. Mutat Res. 2003; 533(1-2) : 153 -71
Cherayil BJ. Iron and immunity: immunological consequences of iron deficiency and overload. Arch Immunol Ther Exp (Warsz). 2010; 58(6) : 407 -15
Bird CL, Witte JS, Swendseid ME, Shikany JM, Hunt IF, Frankl HD, et al. Plasma ferritin, iron intake, and the risk of colorectal polyps. Am J Epidemiol. 1996; 144(1) : 34 -41
Huang X. Does iron have a role in breast cancer? Lancet Oncol. 2008; 9(8) : 803 -7
Jian J, Pelle E, Huang X. Iron and menopause: does increased iron affect the health of postmenopausal women? Antioxid Redox Signal. 2009; 11(12) : 2939 -43
Geissler C, Singh M. Iron, meat and health. Nutrients. 2011; 3(3) : 283 -316
Connor JR, Lee SY. Iron and Cancer. 2010; : 469 -96
Kovacevic Z, Kalinowski DS, Lovejoy DB, Yu Y, Suryo Rahmanto Y, Sharpe PC, et al. The medicinal chemistry of novel iron chelators for the treatment of cancer. Curr Top Med Chem. 2011; 11(5) : 483 -99
Foy SP, Labhasetwar V. Oh the irony: Iron as a cancer cause or cure? Biomaterials. 2011; 32(35) : 9155 -8
Choi JY, Neuhouser ML, Barnett MJ, Hong CC, Kristal AR, Thornquist MD, et al. Iron intake, oxidative stress-related genes (MnSOD and MPO) and prostate cancer risk in CARET cohort. Carcinogenesis. 2008; 29(5) : 964 -70
Alberts DS, Lluria-Prevatt M, Foreword MJA, Romagnolo DF. Bioactive compounds and cancer. 2010;
Kabat GC, Rohan TE. Does excess iron play a role in breast carcinogenesis? An unresolved hypothesis. Cancer Causes Control. 2007; 18(10) : 1047 -53
Toyokuni S. Mysterious link between iron overload and CDKN2A/2B. J Clin Biochem Nutr. 2011; 48(1) : 46 -9
Storz P. Reactive oxygen species in tumor progression. Front Biosci. 2005; 10 : 1881 -96
Valko M, Rhodes CJ, Moncol J, Izakovic M, Mazur M. Free radicals, metals and antioxidants in oxidative stress-induced cancer. Chem Biol Interact. 2006; 160(1) : 1 -40
Munoz M, Villar I, Garcia-Erce JA. An update on iron physiology. World J Gastroenterol. 2009; 15(37) : 4617 -26
Cross AJ, Ferrucci LM, Risch A, Graubard BI, Ward MH, Park Y, et al. A large prospective study of meat consumption and colorectal cancer risk: an investigation of potential mechanisms underlying this association. Cancer Res. 2010; 70(6) : 2406 -14
Daniel CR, Cross AJ, Graubard BI, Hollenbeck AR, Park Y, Sinha R. Prospective investigation of poultry and fish intake in relation to cancer risk. Cancer Prev Res (Phila). 2011; 4(11) : 1903 -11
Corpet DE. Red meat and colon cancer: should we become vegetarians, or can we make meat safer? Meat Sci. 2011; 89(3) : 310 -6
Balder HF, Vogel J, Jansen MC, Weijenberg MP, van den Brandt PA, Westenbrink S, et al. Heme and chlorophyll intake and risk of colorectal cancer in the Netherlands cohort study. Cancer Epidemiol Biomarkers Prev. 2006; 15(4) : 717 -25
Luqman M, Javed MM, Daud S, Raheem N, Ahmad J, Khan AU. Risk factors for lung cancer in the Pakistani population. Asian Pac J Cancer Prev. 2014; 15(7) : 3035 -9
Tasevska N, Sinha R, Kipnis V, Subar AF, Leitzmann MF, Hollenbeck AR, et al. A prospective study of meat, cooking methods, meat mutagens, heme iron, and lung cancer risks. Am J Clin Nutr. 2009; 89(6) : 1884 -94
Pierre F, Freeman A, Tache S, Van der Meer R, Corpet DE. Beef meat and blood sausage promote the formation of azoxymethane-induced mucin-depleted foci and aberrant crypt foci in rat colons. J Nutr. 2004; 134(10) : 2711 -6
Sesink AL, Termont DS, Kleibeuker JH, Van der Meer R. Red meat and colon cancer: the cytotoxic and hyperproliferative effects of dietary heme. Cancer Res. 1999; 59(22) : 5704 -9
Ilsley JN, Belinsky GS, Guda K, Zhang Q, Huang X, Blumberg JB, et al. Dietary iron promotes azoxymethane-induced colon tumors in mice. Nutr Cancer. 2004; 49(2) : 162 -9
Ferrucci LM, Sinha R, Ward MH, Graubard BI, Hollenbeck AR, Kilfoy BA, et al. Meat and components of meat and the risk of bladder cancer in the NIH-AARP Diet and Health Study. Cancer. 2010; 116(18) : 4345 -53
Loh YH, Jakszyn P, Luben RN, Mulligan AA, Mitrou PN, Khaw KT. N-Nitroso compounds and cancer incidence: the European Prospective Investigation into Cancer and Nutrition (EPIC)-Norfolk Study. Am J Clin Nutr. 2011; 93(5) : 1053 -61
Cross AJ, Pollock JR, Bingham SA. Haem, not protein or inorganic iron, is responsible for endogenous intestinal N-nitrosation arising from red meat. Cancer Res. 2003; 63(10) : 2358 -60
Kuhnle GGC, Bingham SA. Meats, Protein and Cancer. 2010; : 195 -212
Lotrean LM, Ailoaiei R, Torres GM. Health risk behavior of Romanian adults having relatives with cancer. Asian Pac J Cancer Prev. 2013; 14(11) : 6465 -8
Pierre F, Peiro G, Tache S, Cross AJ, Bingham SA, Gasc N, et al. New marker of colon cancer risk associated with heme intake: 1,4-dihydroxynonane mercapturic acid. Cancer Epidemiol Biomarkers Prev. 2006; 15(11) : 2274 -9
Kabat GC, Cross AJ, Park Y, Schatzkin A, Hollenbeck AR, Rohan TE, et al. Intakes of dietary iron and heme-iron and risk of postmenopausal breast cancer in the National Institutes of Health-AARP Diet and Health Study. Am J Clin Nutr. 2010; 92(6) : 1478 -83
Ferrucci LM, Cross AJ, Graubard BI, Brinton LA, McCarty CA, Ziegler RG, et al. Intake of meat, meat mutagens, and iron and the risk of breast cancer in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. Br J Cancer. 2009; 101(1) : 178 -84
Kabat GC, Miller AB, Jain M, Rohan TE. Dietary iron and heme iron intake and risk of breast cancer: a prospective cohort study. Cancer Epidemiol Biomarkers Prev. 2007; 16(6) : 1306 -8
Kallianpur AR, Lee SA, Gao YT, Lu W, Zheng Y, Ruan ZX, et al. Dietary animal-derived iron and fat intake and breast cancer risk in the Shanghai Breast Cancer Study. Breast Cancer Res Treat. 2008; 107(1) : 123 -32
Kabat GC, Miller AB, Jain M, Rohan TE. Dietary iron and haem iron intake and risk of endometrial cancer: a prospective cohort study. Br J Cancer. 2008; 98(1) : 194 -8
Genkinger JM, Friberg E, Goldbohm RA, Wolk A. Long-term dietary heme iron and red meat intake in relation to endometrial cancer risk. Am J Clin Nutr. 2012; 96(4) : 848 -54
Kabat GC, Miller AB, Jain M, Rohan TE. A cohort study of dietary iron and heme iron intake and risk of colorectal cancer in women. Br J Cancer. 2007; 97(1) : 118 -22
Sinha R, Park Y, Graubard BI, Leitzmann MF, Hollenbeck A, Schatzkin A, et al. Meat and meat-related compounds and risk of prostate cancer in a large prospective cohort study in the United States. Am J Epidemiol. 2009; 170(9) : 1165 -77
Noto JM, Gaddy JA, Lee JY, Piazuelo MB, Friedman DB, Colvin DC, et al. Iron deficiency accelerates Helicobacter pylori-induced carcinogenesis in rodents and humans. J Clin Invest. 2013; 123(1) : 479 -92
Santarelli RL, Pierre F, Corpet DE. Processed meat and colorectal cancer: a review of epidemiologic and experimental evidence. Nutr Cancer. 2008; 60(2) : 131 -44
Santarelli RL, Vendeuvre JL, Naud N, Tache S, Gueraud F, Viau M, et al. Meat processing and colon carcinogenesis: cooked, nitrite-treated, and oxidized high-heme cured meat promotes mucin-depleted foci in rats. Cancer Prev Res (Phila). 2010; 3(7) : 852 -64
Sinha R, Peters U, Cross AJ, Kulldorff M, Weissfeld JL, Pinsky PF, et al. Meat, meat cooking methods and preservation, and risk for colorectal adenoma. Cancer Res. 2005; 65(17) : 8034 -41
Zheng W, Lee SA. Well-done meat intake, heterocyclic amine exposure, and cancer risk. Nutr Cancer. 2009; 61(4) : 437 -46
Alaejos MS, Afonso AM. Factors that affect the content of heterocyclic aromatic amines in foods. Compr Rev Food Sci Food Saf. 2011; 10(2) : 52 -108
Lakshmi VM, Hsu FF, Zenser TV. Nitric oxide-mediated nitrosation of 2-amino-3,8-dimethylimidazo[4,5-f]quinoxaline potentiated by hemin and myeloperoxidase. Chem Res Toxicol. 2005; 18(6) : 1038 -47
Lakshmi VM, Clapper ML, Chang WC, Zenser TV. Hemin potentiates nitric oxide-mediated nitrosation of 2-amino-3-methylimidazo[4,5-f]quinoline (IQ) to 2-nitrosoamino-3-methylimidazo[4,5-f]quinoline. Chem Res Toxicol. 2005; 18(3) : 528 -35
Yuste J, Mor-Mur M, Capellas M, Guamis B, Pla R. Mechanically recovered poultry meat sausages manufactured with high hydrostatic pressure. Poult Sci. 1999; 78(6) : 914 -21
Ma H, Ledward DA. High pressure processing of fresh meat--is it worth it? Meat Sci. 2013; 95(4) : 897 -903
Cross AJ, Sinha R, Wood RJ, Xue X, Huang WY, Yeager M, et al. Iron homeostasis and distal colorectal adenoma risk in the prostate, lung, colorectal, and ovarian cancer screening trial. Cancer Prev Res (Phila). 2011; 4(9) : 1465 -75
Kesavan Y, Giovannucci E, Fuchs CS, Michaud DS. A prospective study of magnesium and iron intake and pancreatic cancer in men. Am J Epidemiol. 2010; 171(2) : 233 -41
Levi F, Pasche C, Lucchini F, La Vecchia C. Dietary intake of selected micronutrients and breast-cancer risk. Int J Cancer. 2001; 91(2) : 260 -3
Payandeh M, Khodarahmi R, Sadeghi M, Sadeghi E. Appearance of Acute Myelogenous Leukemia (AML) in a Patient with Breast Cancer after Adjuvant Chemotherapy: Case Report and Review of the Literature. Iran J Cancer Prev. 2015; 8(2) : 125 -8
Abraham BK, Justenhoven C, Pesch B, Harth V, Weirich G, Baisch C, et al. Investigation of genetic variants of genes of the hemochromatosis pathway and their role in breast cancer. Cancer Epidemiol Biomarkers Prev. 2005; 14(5) : 1102 -7
Jian J, Yang Q, Dai J, Eckard J, Axelrod D, Smith J, et al. Effects of iron deficiency and iron overload on angiogenesis and oxidative stress-a potential dual role for iron in breast cancer. Free Radic Biol Med. 2011; 50(7) : 841 -7
Bae YJ, Yeon JY, Sung CJ, Kim HS, Sung MK. Dietary intake and serum levels of iron in relation to oxidative stress in breast cancer patients. J Clin Biochem Nutr. 2009; 45(3) : 355 -60
Lee DH, Anderson KE, Harnark LJ, Jacobs DR. Dietary iron intake and breast cancer: The iowa women's heath study. Proc Am Assoc Cancer Res. 2004; 45(1) : 535
Adzersen KH, Jess P, Freivogel KW, Gerhard I, Bastert G. Raw and cooked vegetables, fruits, selected micronutrients, and breast cancer risk: a case-control study in Germany. Nutr Cancer. 2003; 46(2) : 131 -7
Huang X, Katz S. Intakes of dietary iron and heme-iron and risk of postmenopausal breast cancer in the National Institutes of Health-AARP Diet and Health Study. Am J Clin Nutr. 2011; 94(2) : 613 -4
Hong CC, Ambrosone CB, Ahn J, Choi JY, McCullough ML, Stevens VL, et al. Genetic variability in iron-related oxidative stress pathways (Nrf2, NQ01, NOS3, and HO-1), iron intake, and risk of postmenopausal breast cancer. Cancer Epidemiol Biomarkers Prev. 2007; 16(9) : 1784 -94
Kallianpur AR, Hall LD, Yadav M, Christman BW, Dittus RS, Haines JL, et al. Increased prevalence of the HFE C282Y hemochromatosis allele in women with breast cancer. Cancer Epidemiol Biomarkers Prev. 2004; 13(2) : 205 -12
Beckman LE, Van Landeghem GF, Sikstrom C, Wahlin A, Markevarn B, Hallmans G, et al. Interaction between haemochromatosis and transferrin receptor genes in different neoplastic disorders. Carcinogenesis. 1999; 20(7) : 1231 -3
Cujic, D. , Stefanoska, I. , Golubovic, S. . Serum ferritin in healthy women and breast cancer patients. J Med Biochem . 2011; 30(1) : 33 -7
Lund EK, Wharf SG, Fairweather-Tait SJ, Johnson IT. Oral ferrous sulfate supplements increase the free radical-generating capacity of feces from healthy volunteers. Am J Clin Nutr. 1999; 69(2) : 250 -5
Keshtkar A, Semnani SH, Besharat S, Aboomardani M, Abdolahi N, Roshandel GH, et al. Colorectal cancer nutritional risk factors: A population based case-control study. Iran J Cancer Prev. 2012; 3(2) : 93 -7
Butterworth JR. Another important function for an old friend! The role of iron in colorectal carcinogenesis. Gut. 2006; 55(10) : 1384 -6
Chua AC, Klopcic B, Lawrance IC, Olynyk JK, Trinder D. Iron: an emerging factor in colorectal carcinogenesis. World J Gastroenterol. 2010; 16(6) : 663 -72
Qiao L, Feng Y. Intakes of heme iron and zinc and colorectal cancer incidence: a meta-analysis of prospective studies. Cancer Causes Control. 2013; 24(6) : 1175 -83
Lund EK, Wharf SG, Fairweather-Tait SJ, Johnson IT. Increases in the concentrations of available iron in response to dietary iron supplementation are associated with changes in crypt cell proliferation in rat large intestine. J Nutr. 1998; 128(2) : 175 -9
Lund EK, Fairweather-Tait SJ, Wharf SG, Johnson IT. Chronic exposure to high levels of dietary iron fortification increases lipid peroxidation in the mucosa of the rat large intestine. J Nutr. 2001; 131(11) : 2928 -31
Armstrong B, Doll R. Environmental factors and cancer incidence and mortality in different countries, with special reference to dietary practices. Int J Cancer. 1975; 15(4) : 617 -31
Bastide NM, Pierre FH, Corpet DE. Heme iron from meat and risk of colorectal cancer: a meta-analysis and a review of the mechanisms involved. Cancer Prev Res (Phila). 2011; 4(2) : 177 -84
Hara A, Sasazuki S, Inoue M, Iwasaki M, Shimazu T, Sawada N, et al. Zinc and heme iron intakes and risk of colorectal cancer: a population-based prospective cohort study in Japan. Am J Clin Nutr. 2012; 96(4) : 864 -73
Zhang X, Giovannucci EL, Smith-Warner SA, Wu K, Fuchs CS, Pollak M, et al. A prospective study of intakes of zinc and heme iron and colorectal cancer risk in men and women. Cancer Causes Control. 2011; 22(12) : 1627 -37
Ashmore JH, Lesko SM, Miller PE, Cross AJ, Muscat JE, Zhu J, et al. Association of dietary and supplemental iron and colorectal cancer in a population-based study. Eur J Cancer Prev. 2013; 22(6) : 506 -11
Wurzelmann JI, Silver A, Schreinemachers DM, Sandler RS, Everson RB. Iron intake and the risk of colorectal cancer. Cancer Epidemiol Biomarkers Prev. 1996; 5(7) : 503 -7
Chan AT, Ma J, Tranah GJ, Giovannucci EL, Rifai N, Hunter DJ, et al. Hemochromatosis gene mutations, body iron stores, dietary iron, and risk of colorectal adenoma in women. J Natl Cancer Inst. 2005; 97(12) : 917 -26
Knekt P, Reunanen A, Takkunen H, Aromaa A, Heliovaara M, Hakulinen T. Body iron stores and risk of cancer. Int J Cancer. 1994; 56(3) : 379 -82
Kuvibidila SR, Gauthier T, Rayford W. Serum ferritin levels and transferrin saturation in men with prostate cancer. J Natl Med Assoc. 2004; 96(5) : 641 -9
Hercberg S, Estaquio C, Czernichow S, Mennen L, Noisette N, Bertrais S, et al. Iron status and risk of cancers in the SU.VI.MAX cohort. J Nutr. 2005; 135(11) : 2664 -8
Nomura A, Chyou PH, Stemmermann GN. Association of serum ferritin levels with the risk of stomach cancer. Cancer Epidemiol Biomarkers Prev. 1992; 1(7) : 547 -50
Stevens RG, Morris JE, Cordis GA, Anderson LE, Rosenberg DW, Sasser LB. Oxidative damage in colon and mammary tissue of the HFE-knockout mouse. Free Radic Biol Med. 2003; 34(9) : 1212 -6
Osborne NJ, Gurrin LC, Allen KJ, Constantine CC, Delatycki MB, McLaren CE, et al. HFE C282Y homozygotes are at increased risk of breast and colorectal cancer. Hepatology. 2010; 51(4) : 1311 -8
Nelson RL, Davis FG, Persky V, Becker E. Risk of neoplastic and other diseases among people with heterozygosity for hereditary hemochromatosis. Cancer. 1995; 76(5) : 875 -9
Ekblom K, Marklund SL, Palmqvist R, Van Guelpen B, Hallmans G, Weinehall L, et al. Iron biomarkers in plasma, HFE genotypes, and the risk for colorectal cancer in a prospective setting. Dis Colon Rectum. 2012; 55(3) : 337 -44
Nelson RL, Davis FG, Sutter E, Sobin LH, Kikendall JW, Bowen P. Body iron stores and risk of colonic neoplasia. J Natl Cancer Inst. 1994; 86(6) : 455 -60
Lee DH, Anderson KE, Harnack LJ, Folsom AR, Jacobs DJ. Heme iron, zinc, alcohol consumption, and colon cancer: Iowa Women's Health Study. J Natl Cancer Inst. 2004; 96(5) : 403 -7
Bothwell TH, MacPhail AP. Hereditary hemochromatosis: etiologic, pathologic, and clinical aspects. Semin Hematol. 1998; 35(1) : 55 -71
Simcox JA, McClain DA. Iron and diabetes risk. Cell Metab. 2013; 17(3) : 329 -41
Forouhi NG, Harding AH, Allison M, Sandhu MS, Welch A, Luben R, et al. Elevated serum ferritin levels predict new-onset type 2 diabetes: results from the EPIC-Norfolk prospective study. Diabetologia. 2007; 50(5) : 949 -56
Rajpathak SN, Wylie-Rosett J, Gunter MJ, Negassa A, Kabat GC, Rohan TE, et al. Biomarkers of body iron stores and risk of developing type 2 diabetes. Diabetes Obes Metab. 2009; 11(5) : 472 -9
Ben Q, Xu M, Ning X, Liu J, Hong S, Huang W, et al. Diabetes mellitus and risk of pancreatic cancer: A meta-analysis of cohort studies. Eur J Cancer. 2011; 47(13) : 1928 -37
Molina-Montes E, Wark PA, Sanchez MJ, Norat T, Jakszyn P, Lujan-Barroso L, et al. Dietary intake of iron, heme-iron and magnesium and pancreatic cancer risk in the European prospective investigation into cancer and nutrition cohort. Int J Cancer. 2012; 131(7) -47
Montonen J, Boeing H, Steffen A, Lehmann R, Fritsche A, Joost HG, et al. Body iron stores and risk of type 2 diabetes: results from the European Prospective Investigation into Cancer and Nutrition (EPIC)-Potsdam study. Diabetologia. 2012; 55(10) : 2613 -21
Lee DH, Folsom AR, Jacobs DJ. Dietary iron intake and Type 2 diabetes incidence in postmenopausal women: the Iowa Women's Health Study. Diabetologia. 2004; 47(2) : 185 -94
Jiang R, Ma J, Ascherio A, Stampfer MJ, Willett WC, Hu FB. Dietary iron intake and blood donations in relation to risk of type 2 diabetes in men: a prospective cohort study. Am J Clin Nutr. 2004; 79(1) : 70 -5
Rajpathak S, Ma J, Manson J, Willett WC, Hu FB. Iron intake and the risk of type 2 diabetes in women: a prospective cohort study. Diabetes Care. 2006; 29(6) : 1370 -6
Olsen GW, Mandel JS, Gibson RW, Wattenberg LW, Schuman LM. Nutrients and pancreatic cancer: a population-based case-control study. Cancer Causes Control. 1991; 2(5) : 291 -7
Baghurst PA, McMichael AJ, Slavotinek AH, Baghurst KI, Boyle P, Walker AM. A case-control study of diet and cancer of the pancreas. Am J Epidemiol. 1991; 134(2) : 167 -79
Ghadirian P, Simard A, Baillargeon J, Maisonneuve P, Boyle P. Nutritional factors and pancreatic cancer in the francophone community in Montreal, Canada. Int J Cancer. 1991; 47(1) : 1 -6
Silverman DT, Swanson CA, Gridley G, Wacholder S, Greenberg RS, Brown LM, et al. Dietary and nutritional factors and pancreatic cancer: a case-control study based on direct interviews. J Natl Cancer Inst. 1998; 90(22) : 1710 -9
Lin Y, Tamakoshi A, Hayakawa T, Naruse S, Kitagawa M, Ohno Y. Nutritional factors and risk of pancreatic cancer: a population-based case-control study based on direct interview in Japan. J Gastroenterol. 2005; 40(3) : 297 -301
Bravi F, Polesel J, Bosetti C, Talamini R, Negri E, Dal Maso L, et al. Dietary intake of selected micronutrients and the risk of pancreatic cancer: an Italian case-control study. Ann Oncol. 2011; 22(1) : 202 -6
Michaud DS, Giovannucci E, Willett WC, Colditz GA, Fuchs CS. Dietary meat, dairy products, fat, and cholesterol and pancreatic cancer risk in a prospective study. Am J Epidemiol. 2003; 157(12) : 1115 -25
Heinen MM, Verhage BA, Goldbohm RA, van den Brandt PA. Meat and fat intake and pancreatic cancer risk in the Netherlands Cohort Study. Int J Cancer. 2009; 125(5) : 1118 -26
Friedman GD, van den Eeden SK. Risk factors for pancreatic cancer: an exploratory study. Int J Epidemiol. 1993; 22(1) : 30 -7
Dongiovanni P, Fracanzani AL, Cairo G, Megazzini CP, Gatti S, Rametta R, et al. Iron-dependent regulation of MDM2 influences p53 activity and hepatic carcinogenesis. Am J Pathol. 2010; 176(2) : 1006 -17
Evangelista AS, Nakhle MC, de Araujo TF, Abrantes-Lemos CP, Deguti MM, Carrilho FJ, et al. HFE genotyping in patients with elevated serum iron indices and liver diseases. Biomed Res Int. 2015; 2015 : 164671
Sebastiani G, Walker AP. HFE gene in primary and secondary hepatic iron overload. World J Gastroenterol. 2007; 13(35) : 4673 -89
Kew MC. Hepatic iron overload and hepatocellular carcinoma. Cancer Lett. 2009; 286(1) : 38 -43
Marrogi AJ, Khan MA, van Gijssel HE, Welsh JA, Rahim H, Demetris AJ, et al. Oxidative stress and p53 mutations in the carcinogenesis of iron overload-associated hepatocellular carcinoma. J Natl Cancer Inst. 2001; 93(21) : 1652 -5
Grando-Lemaire V, Guettier C, Chevret S, Beaugrand M, Trinchet JC. Hepatocellular carcinoma without cirrhosis in the West: epidemiological factors and histopathology of the non-tumorous liver. Groupe d'Etude et de Traitement du Carcinome Hepatocellulaire. J Hepatol. 1999; 31(3) : 508 -13
Hann HW, Kim CY, London WT, Blumberg BS. Increased serum ferritin in chronic liver disease: a risk factor for primary hepatocellular carcinoma. Int J Cancer. 1989; 43(3) : 376 -9
Ko C, Siddaiah N, Berger J, Gish R, Brandhagen D, Sterling RK, et al. Prevalence of hepatic iron overload and association with hepatocellular cancer in end-stage liver disease: results from the National Hemochromatosis Transplant Registry. Liver Int. 2007; 27(10) : 1394 -401
Gordeuk VR, McLaren CE, MacPhail AP, Deichsel G, Bothwell TH. Associations of iron overload in Africa with hepatocellular carcinoma and tuberculosis: Strachan's 1929 thesis revisited. Blood. 1996; 87(8) : 3470 -6
Mandishona E, MacPhail AP, Gordeuk VR, Kedda MA, Paterson AC, Rouault TA, et al. Dietary iron overload as a risk factor for hepatocellular carcinoma in Black Africans. Hepatology. 1998; 27(6) : 1563 -6
Moyo VM, Makunike R, Gangaidzo IT, Gordeuk VR, McLaren CE, Khumalo H, et al. African iron overload and hepatocellular carcinoma (HA-7-0-080). Eur J Haematol. 1998; 60(1) : 28 -34
Gangaidzo IT, Gordeuk VR. Hepatocellular carcinoma and African iron overload. Gut. 1995; 37(5) : 727 -30
Gordeuk V, Mukiibi J, Hasstedt SJ, Samowitz W, Edwards CQ, West G, et al. Iron overload in Africa. Interaction between a gene and dietary iron content. N Engl J Med. 1992; 326(2) : 95 -100
Kato J, Kobune M, Kohgo Y, Sugawara N, Hisai H, Nakamura T, et al. Hepatic iron deprivation prevents spontaneous development of fulminant hepatitis and liver cancer in Long-Evans Cinnamon rats. J Clin Invest. 1996; 98(4) : 923 -9
Weinberg ED. Iron loading and disease surveillance. Emerg Infect Dis. 1999; 5(3) : 346 -52
Kumar M, Kumar R, Hissar SS, Saraswat MK, Sharma BC, Sakhuja P, et al. Risk factors analysis for hepatocellular carcinoma in patients with and without cirrhosis: a case-control study of 213 hepatocellular carcinoma patients from India. J Gastroenterol Hepatol. 2007; 22(7) : 1104 -11
Khosravi P, Zahiri J, Gazestani VH, Mirkhalaf S, Akbarzadeh M, Sadeghi M, et al. Analysis of candidate genes has proposed the role of y chromosome in human prostate cancer. Iran J Cancer Prev. 2014; 7(4) : 204 -11
Bashir MN, Ahmad MR, Malik A. Risk factors of prostate cancer: a case-control study in Faisalabad, Pakistan. Asian Pac J Cancer Prev. 2014; 15(23) : 10237 -40
Jakszyn PG, Allen NE, Lujan-Barroso L, Gonzalez CA, Key TJ, Fonseca-Nunes A, et al. Nitrosamines and heme iron and risk of prostate cancer in the European prospective investigation into cancer and nutrition. Cancer Epidemiol Biomarkers Prev. 2012; 21(3) : 547 -51
Chen L, Stacewicz-Sapuntzakis M, Duncan C, Sharifi R, Ghosh L, van Breemen R, et al. Oxidative DNA damage in prostate cancer patients consuming tomato sauce-based entrees as a whole-food intervention. J Natl Cancer Inst. 2001; 93(24) : 1872 -9
Tappel A. Heme of consumed red meat can act as a catalyst of oxidative damage and could initiate colon, breast and prostate cancers, heart disease and other diseases. Med Hypotheses. 2007; 68(3) : 562 -4
Ornstein DL, Zacharski LR. Iron stimulates urokinase plasminogen activator expression and activates nf-kappa b in human prostate cancer cells. Nutrition Cancer. 2007; 58(1) : 115 -26
Ma RW, Chapman K. A systematic review of the effect of diet in prostate cancer prevention and treatment. J Hum Nutr Diet. 2009; 22(3) : 187 -99
Kolonel LN. Fat, meat, and prostate cancer. Epidemiol Rev. 2001; 23(1) : 72 -81
Alexander DD, Mink PJ, Cushing CA, Sceurman B. A review and meta-analysis of prospective studies of red and processed meat intake and prostate cancer. Nutr J. 2010; 9 : 50
Nicastro HL, Dunn BK. Selenium and prostate cancer prevention: insights from the selenium and vitamin E cancer prevention trial (SELECT). Nutrients. 2013; 5(4) : 1122 -48
Matos HR, Marques SA, Gomes OF, Silva AA, Heimann JC, Di Mascio P, et al. Lycopene and beta-carotene protect in vivo iron-induced oxidative stress damage in rat prostate. Braz J Med Biol Res. 2006; 39(2) : 203 -10
Stevens RG, Graubard BI, Micozzi MS, Neriishi K, Blumberg BS. Moderate elevation of body iron level and increased risk of cancer occurrence and death. Int J Cancer. 1994; 56(3) : 364 -9
Kuvibidila S, Gauthier T, Warrier RP, Rayford W. Increased levels of serum transferrin receptor and serum transferrin receptor/log ferritin ratios in men with prostate cancer and the implications for body-iron stores. J Lab Clin Med. 2004; 144(4) : 176 -82
Tandon VR, Sharma S, Mahajan A, Bardi GH. Oxidative stress: a novel strategy in cancer treatment. . J K Sci. 2005; 7(1) : 48
Miguel M, Cordero MD. Oxidative therapy against cancer. 2012;
Amirijavid S, Hashemi M. Detection of Anticancer and Apoptotic Effect of the Produced IgYs against the Three Extracellular Domain of Human DR5 Protein. Iran J Cancer Prev. 2015; 8(2) : 109 -15
Hasegawa Y, Takano T, Miyauchi A, Matsuzuka F, Yoshida H, Kuma K, et al. Decreased expression of glutathione peroxidase mRNA in thyroid anaplastic carcinoma. Cancer Lett. 2002; 182(1) : 69 -74
Pelicano H, Carney D, Huang P. ROS stress in cancer cells and therapeutic implications. Drug Resist Updat. 2004; 7(2) : 97 -110
McCarty MF, Barroso-Aranda J, Contreras F. Oxidative stress therapy for solid tumors - a proposal. Med Hypotheses. 2010; 74(6) : 1052 -4
Ferle-Vidovic A, Poljak-Blazi M, Rapic V, Skare D. Ferrocenes (F168, F169) and fero-sorbitol-citrate (FSC): potential anticancer drugs. Cancer Biother Radiopharm. 2000; 15(6) : 617 -24
Kiessling MK, Klemke CD, Kaminski MM, Galani IE, Krammer PH, Gulow K. Inhibition of constitutively activated nuclear factor-kappaB induces reactive oxygen species- and iron-dependent cell death in cutaneous T-cell lymphoma. Cancer Res. 2009; 69(6) : 2365 -74
Alarifi S, Ali D, Alkahtani S, Alhader MS. Iron oxide nanoparticles induce oxidative stress, DNA damage, and caspase activation in the human breast cancer cell line. Biol Trace Elem Res. 2014; 159(1-3) : 416 -24
Gumienna-Kontecka E, Pyrkosz-Bulska M, Szebesczyk A, Ostrowska M. Iron chelating strategies in systemic metal overload, neurodegeneration and cancer. Curr Med Chem. 2014; 21(33) : 3741 -67
Jiao Y, Wilkinson J, Di X, Wang W, Hatcher H, Kock ND, et al. Curcumin, a cancer chemopreventive and chemotherapeutic agent, is a biologically active iron chelator. Blood. 2009; 113(2) : 462 -9
Saletta F, Kovacevic Z, Richardson DR. Iron chelation: deciphering novel molecular targets for cancer therapy. The tip of the iceberg of a web of iron-regulated molecules. Future Med Chem. 2011; 3(16) : 1983 -6
Jiao Y, Wilkinson J, Christine Pietsch E, Buss JL, Wang W, Planalp R, et al. Iron chelation in the biological activity of curcumin. Free Radic Biol Med. 2006; 40(7) : 1152 -60
Bayet-Robert M, Kwiatkowski F, Leheurteur M, Gachon F, Planchat E, Abrial C, et al. Phase I dose escalation trial of docetaxel plus curcumin in patients with advanced and metastatic breast cancer. Cancer Biol Ther. 2010; 9(1) : 8 -14
Tavakoli J, Miar S, Majid Zadehzare M, Akbari H. Evaluation of effectiveness of herbal medication in cancer care: a review study. Iran J Cancer Prev. 2012; 5(3) : 144 -56
Minear S, O'Donnell AF, Ballew A, Giaever G, Nislow C, Stearns T, et al. Curcumin inhibits growth of Saccharomyces cerevisiae through iron chelation. Eukaryot Cell. 2011; 10(11) : 1574 -81
Du XX, Xu HM, Jiang H, Song N, Wang J, Xie JX. Curcumin protects nigral dopaminergic neurons by iron-chelation in the 6-hydroxydopamine rat model of Parkinson's disease. Neurosci Bull. 2012; 28(3) : 253 -8
Hutchinson C, Bomford A, Geissler CA. The iron-chelating potential of silybin in patients with hereditary haemochromatosis. Eur J Clin Nutr. 2010; 64(10) : 1239 -41
Kauntz H, Bousserouel S, Gosse F, Marescaux J, Raul F. Silibinin, a natural flavonoid, modulates the early expression of chemoprevention biomarkers in a preclinical model of colon carcinogenesis. Int J Oncol. 2012; 41(3) : 849 -54
Raina K, Rajamanickam S, Singh RP, Deep G, Chittezhath M, Agarwal R. Stage-specific inhibitory effects and associated mechanisms of silibinin on tumor progression and metastasis in transgenic adenocarcinoma of the mouse prostate model. Cancer Res. 2008; 68(16) : 6822 -30
Bares JM, Berger J, Nelson JE, Messner DJ, Schildt S, Standish LJ, et al. Silybin treatment is associated with reduction in serum ferritin in patients with chronic hepatitis C. J Clin Gastroenterol. 2008; 42(8) : 937 -44
Vaid M, Katiyar SK. Molecular mechanisms of inhibition of photocarcinogenesis by silymarin, a phytochemical from milk thistle (Silybum marianum L. Gaertn.) (Review). Int J Oncol. 2010; 36(5) : 1053 -60
Bhasin G, Kausar H, Sarwar Alam M, Athar M. Progressive iron overload enhances chemically mediated tumor promotion in murine skin. Arch Biochem Biophys. 2003; 409(2) : 262 -73
Zacharski LR, Chow BK, Howes PS, Shamayeva G, Baron JA, Dalman RL, et al. Decreased cancer risk after iron reduction in patients with peripheral arterial disease: results from a randomized trial. J Natl Cancer Inst. 2008; 100(14) : 996 -1002
Merk K, Mattsson B, Mattsson A, Holm G, Gullbring B, Bjorkholm M. The incidence of cancer among blood donors. Int J Epidemiol. 1990; 19(3) : 505 -9
Edgren G, Reilly M, Hjalgrim H, Tran TN, Rostgaard K, Adami J, et al. Donation frequency, iron loss, and risk of cancer among blood donors. J Natl Cancer Inst. 2008; 100(8) : 572 -9
World Health Organization. . Micronutrient deficiencies. Iron deficiency anemia.
Nutritional and safety assessments of foods and feeds nutritionally improved through biotechnology: An executive summary a task force report by the international life sciences institute, Washington, D.C. Compr Rev Food Sci Food Saf. 2004; 3(2) : 35 -104
Pra D, Rech Franke SI, Pegas Henriques JA, Fenech M. A possible link between iron deficiency and gastrointestinal carcinogenesis. Nutr Cancer. 2009; 61(4) : 415 -26
Dallman PR. Iron deficiency and the immune response. Am J Clin Nutr. 1987; 46(2) : 329 -34
Lockwood JF, Sherman AR. Spleen natural killer cells from iron-deficient rat pups manifest an altered ability to be stimulated by interferon. J Nutr. 1988; 118(12) : 1558 -63
Spear AT, Sherman AR. Iron deficiency alters DMBA-induced tumor burden and natural killer cell cytotoxicity in rats. J Nutr. 1992; 122(1) : 46 -55
Kuvibidila SR, Velez M, Gardner R, Penugonda K, Chandra LC, Yu L. Iron deficiency reduces serum and in vitro secretion of interleukin-4 in mice independent of altered spleen cell proliferation. Nutr Res. 2012; 32(2) : 107 -15
Langers I, Renoux VM, Thiry M, Delvenne P, Jacobs N. Natural killer cells: role in local tumor growth and metastasis. Biologics. 2012; 6 : 73 -82
Bredenkamp JK, Castro DJ, Mickel RA. Importance of iron repletion in the management of Plummer-Vinson syndrome. Ann Otol Rhinol Laryngol. 1990; 99(1) : 51 -4
Tabatabaei SA, Hashemi SM, Kelidari B. Transhiatal Esophagectomy without Mediastinal Manipulation for Lower Third Esophageal and Cardial Cancers: The First Experience of a New Technique. Iran J Cancer Prev. 2015; 8(2) : 89 -93
Kim KH, Kim MC, Jung GJ. Gastric cancer occurring in a patient with Plummer-Vinson syndrome: a case report. World J Gastroenterol. 2005; 11(44) : 7048 -50
Broitman SA, Velez H, Vitale JJ. A possible role of iron deficiency in gastric cancer in Colombia. Adv Exp Med Biol. 1981; 135 : 155 -81
Zhang YW, Eom SY, Kim YD, Song YJ, Yun HY, Park JS, et al. Effects of dietary factors and the NAT2 acetylator status on gastric cancer in Koreans. Int J Cancer. 2009; 125(1) : 139 -45
Richie JJ, Kleinman W, Marina P, Abraham P, Wynder EL, Muscat JE. Blood iron, glutathione, and micronutrient levels and the risk of oral cancer. Nutr Cancer. 2008; 60(4) : 474 -82
Maxwell P, Salnikow K. HIF-1: an oxygen and metal responsive transcription factor. Cancer Biol Ther. 2004; 3(1) : 29 -35
Liu LZ, Jing Y, Jiang LL, Jiang XE, Jiang Y, Rojanasakul Y, et al. Acacetin inhibits VEGF expression, tumor angiogenesis and growth through AKT/HIF-1alpha pathway. Biochem Biophys Res Commun. 2011; 413(2) : 299 -305


.png)